If you’ve been told your thyroid is overactive — or if you’re dealing with a racing heart, unexplained weight loss, shaky hands, or eyes that feel like they’re being pushed forward — Graves’ disease may be behind it. As a board-certified endocrinologist and thyroid specialist serving Fairfield County, CT, I’ve spent over 20 years diagnosing and treating thyroid disorders, and Graves’ disease is one of the conditions I work with most. It’s often misunderstood, frequently undertreated, and far more nuanced than most patients are told.
This post is my attempt to give you a clear, complete picture: what Graves’ disease actually is, why it affects some people and not others, what symptoms to watch for, and what your real treatment options are — both conventional and functional — in 2026. If you’d prefer to skip ahead and talk to someone directly, you can schedule a consultation here.
🎧 Listen to this article
What Is Graves’ Disease?
Graves’ disease is an autoimmune condition — meaning your immune system is attacking your own tissue. In this case, it produces antibodies called thyroid-stimulating immunoglobulins (TSI) that bind to and continuously activate your thyroid-stimulating hormone receptor (TSHR). The result: your thyroid gland gets an unrelenting “on” signal and produces far more thyroid hormone than your body needs.
That excess thyroid hormone throws nearly every system in your body into overdrive. Your heart rate climbs. Your metabolism accelerates. Your nervous system becomes hyperactivated. Left untreated, the downstream consequences — on your heart, bones, and eyes — can be serious and lasting.
Graves’ disease is the most common cause of hyperthyroidism, responsible for 60–80% of all hyperthyroid cases. It predominantly affects women, particularly those of reproductive age, at a rate roughly 5 to 10 times higher than men. But it can and does affect men, older adults, and people across all demographics — which is why getting the right diagnosis matters so much.
Graves’ Disease vs. Hashimoto’s: Understanding the Difference
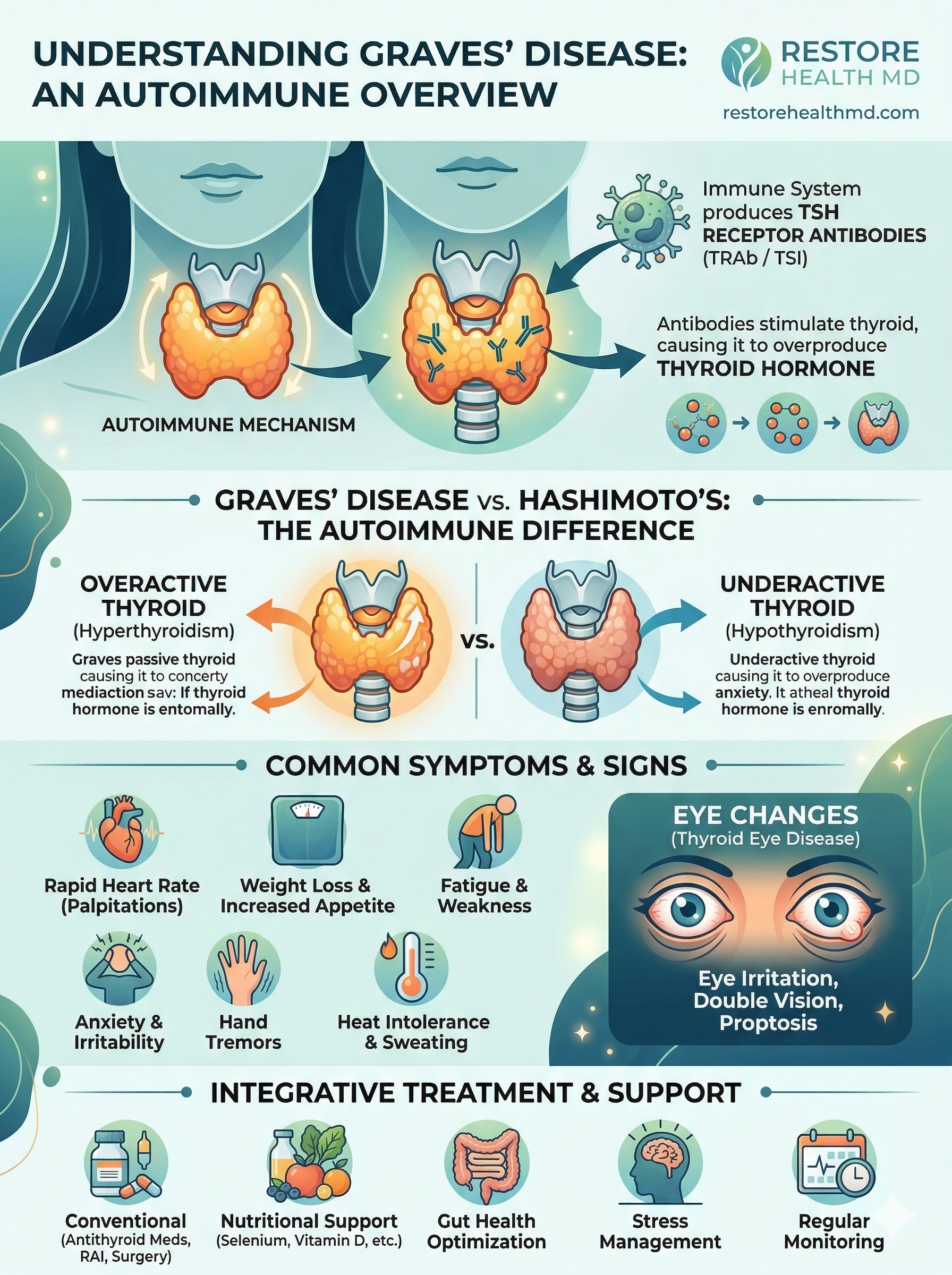
Patients often confuse Graves’ disease with Hashimoto’s thyroiditis because both are autoimmune thyroid conditions. But they work in opposite directions.
Hashimoto’s predominantly causes the immune system to gradually destroy thyroid tissue, leading to an underactive thyroid (hypothyroidism) — fatigue, weight gain, cold intolerance, brain fog. However, there is an important nuance: during flares of active thyroid inflammation (a process called Hashitoxicosis), damaged thyroid cells can release a surge of stored thyroid hormone into the bloodstream, causing a period of transient hyperthyroidism. This typically resolves on its own as the inflammation settles — but it can look and feel exactly like Graves’ disease, which is why antibody testing is so critical. Treating Hashitoxicosis with antithyroid drugs or radioactive iodine would be the wrong call entirely.
Graves’ disease causes the immune system to continuously overstimulate the thyroid via TSI antibodies, producing a sustained overactive thyroid state — racing heart, weight loss, heat intolerance, anxiety, and more. Unlike Hashimoto’s-related hyperthyroidism, this doesn’t resolve on its own without treatment.
In some cases, a person can have features of both conditions simultaneously. This is part of why I never treat a thyroid condition based on symptoms alone — proper antibody testing and thyroid function labs are essential to get the diagnosis right before deciding on treatment.
Signs and Symptoms of Graves’ Disease
Because excess thyroid hormone accelerates virtually every metabolic process in your body, the symptom list for Graves’ disease is wide-ranging. The most common ones I see in my Fairfield, CT practice include:
- Rapid or irregular heartbeat (palpitations)
- Unintentional weight loss despite a normal or increased appetite
- Heat intolerance and excessive sweating
- Tremor (most often in the hands and fingers)
- Anxiety, nervousness, and irritability
- Fatigue and muscle weakness
- Frequent bowel movements
- Irregular menstrual cycles in women
- Difficulty sleeping
- Enlarged thyroid gland (goiter) — a visible or palpable swelling in the neck
There are also two manifestations that are specific to Graves’ disease and don’t occur with other causes of hyperthyroidism:
Graves’ Ophthalmopathy (Thyroid Eye Disease)
Estimates vary, but studies suggest that roughly 25–40% of patients with Graves’ disease develop some degree of thyroid eye disease (TED) — an inflammatory condition affecting the tissues and muscles behind the eyes. It’s important to understand that TED exists on a spectrum. The majority of cases are mild, presenting with dry or gritty eyes, lid retraction, or subtle puffiness around the eyes. Only a smaller subset — perhaps 5–6% — develop moderate-to-severe disease with significant eye bulging (proptosis), double vision, or vision-threatening complications. That distinction matters, because mild TED is often overlooked entirely unless your provider is specifically screening for it. Severe TED deserves aggressive, specialized management — not just monitoring — and that’s true whether you’re symptomatic or not.
Pretibial Myxedema (Graves’ Dermopathy)
A less common but distinctive feature is thickening and reddening of the skin, usually over the shins. It occurs in a small percentage of patients, most often those with more severe disease or significant eye involvement.
How Is Graves’ Disease Diagnosed?
A proper Graves’ disease workup goes beyond a basic thyroid panel. In my practice, I typically order:
- TSH (thyroid-stimulating hormone) — will be suppressed (low) in hyperthyroidism
- Free T4 and Free T3 — elevated in active Graves’ disease
- TSH receptor antibodies (TRAb) / Thyroid-stimulating immunoglobulins (TSI) — the TSI antibody test is the defining marker for Graves’ disease; its presence essentially confirms the diagnosis and distinguishes Graves’ from other causes of hyperthyroidism
- Radioactive iodine uptake scan (RAIU) — when the diagnosis is uncertain, this can help differentiate Graves’ disease from other causes of hyperthyroidism
- Thyroid ultrasound — to assess gland size, vascularity, and rule out nodules
The combination of a suppressed TSH, elevated thyroid hormones, and positive TRAb antibodies is essentially diagnostic. Thyroid eye disease, if present, is also pathognomonic — meaning it’s essentially definitive for Graves’ disease on its own. If you’re unsure what your current labs mean, reach out directly — interpreting a comprehensive thyroid panel is one of the most common things I do at a first visit.
Treatment Options for Graves’ Disease
There is no one-size-fits-all answer for Graves’ disease treatment. The right approach depends on your age, severity of disease, antibody levels, whether you have thyroid eye disease, pregnancy status, and your own preferences. Here’s how I think through the options:
1. Antithyroid Medications (ATDs)
Methimazole (MMI) is currently the preferred first-line treatment for most patients in the United States — a significant shift from the radioactive iodine-dominant approach of prior decades. Methimazole works by blocking thyroid peroxidase, the enzyme responsible for thyroid hormone synthesis. It also appears to have a favorable effect on thyroid autoimmunity itself, potentially contributing to remission over time.
ATDs are well-tolerated when used appropriately. For patients who don’t achieve remission on a standard 12–24 month course, long-term or indefinite ATD therapy is increasingly recognized as a safe and effective option — something I actively discuss with my patients rather than rushing toward more definitive interventions.
Propylthiouracil (PTU) is generally reserved for specific situations — including the first trimester of pregnancy and thyroid storm — due to a higher risk of liver toxicity compared to methimazole.
2. Radioactive Iodine (RAI) Therapy
Radioactive iodine has been used for decades and remains a valid option for many patients. Delivered orally, it’s absorbed selectively by thyroid tissue and gradually destroys overactive thyroid cells. It resolves hyperthyroidism in the majority of patients — but typically results in hypothyroidism, meaning lifelong thyroid hormone replacement afterward.
RAI is not recommended in patients with active, moderate-to-severe thyroid eye disease, as it can worsen the eye condition. I use it selectively, and always with a full informed discussion of what to expect post-treatment.
3. Thyroidectomy
Surgical removal of the thyroid (thyroidectomy) is the fastest way to definitively control Graves’ disease and is the preferred option when the goiter is very large, there is a concern for thyroid cancer, or when rapid normalization is needed — for example, in severe or poorly controlled disease. Like RAI, it results in hypothyroidism requiring lifelong levothyroxine replacement.
When performed by an experienced, high-volume thyroid surgeon, the risks of serious complications — such as nerve injury or parathyroid damage — are low. Choosing the right surgical team matters enormously.
4. Managing Thyroid Eye Disease
Thyroid eye disease requires its own management track. Mild cases are often managed with lubricating eye drops, UV-protective glasses, and selenium supplementation. Moderate-to-severe cases may require:
- IV glucocorticoids
- Orbital radiation
- Teprotumumab (Tepezza) — an FDA-approved IGF-1R inhibitor that has shown significant efficacy in reducing proptosis and improving quality of life in patients with active thyroid eye disease
- Orbital decompression surgery in refractory cases
Emerging targeted therapies — including monoclonal antibodies directed at the TSH receptor and immune pathways like CD20 and CD40 — are currently in active clinical trials and represent a genuinely exciting frontier in Graves’ disease management. These are approaches I follow closely.
Functional Medicine Approaches to Graves’ Disease
Conventional treatment addresses the thyroid directly — but Graves’ disease is an immune system problem that happens to express itself through the thyroid. That distinction matters. As someone who practices at the intersection of endocrinology and functional medicine, I work with patients to identify and address the upstream drivers of immune dysregulation alongside standard treatment. Here are the interventions with the most meaningful evidence behind them:
Selenium
Selenium is the most evidence-backed nutritional intervention in autoimmune thyroid disease. The thyroid has one of the highest selenium concentrations of any tissue in the body, and selenium-dependent enzymes are essential for thyroid hormone metabolism and antioxidant defense. In patients with Graves’ disease, selenium supplementation (typically 200 mcg/day of selenomethionine) has been shown in randomized controlled trials to reduce TRAb antibody levels and improve mild thyroid eye disease — and is recommended by the European Thyroid Association for mild Graves’ ophthalmopathy. I check selenium status before supplementing, as excess selenium carries its own risks.
Vitamin D Optimization
Vitamin D functions more like a hormone than a vitamin, and it plays a significant regulatory role in immune tolerance. Deficiency is consistently associated with higher rates of autoimmune thyroid disease, including Graves’ disease. Optimizing Vitamin D — not just to the conventional lab minimum, but to a functional range of 60–80 ng/mL — is a routine part of my approach to autoimmune thyroid management. It won’t replace antithyroid medication, but it addresses a modifiable immune driver that most conventional workups overlook entirely.
Stress and HPA Axis Regulation
Psychological stress is one of the most consistently identified environmental triggers for Graves’ disease onset and relapse. Stress activates the HPA (hypothalamic-pituitary-adrenal) axis and promotes the immune dysregulation that drives autoimmunity. In practice, this means I address sleep quality, recommend temporary modifications to exercise intensity when the body is under thyroid-related stress, and work through personalized stress management strategies — all as active clinical interventions, not afterthoughts.
Gut Health and Intestinal Permeability
Emerging research continues to link gut microbiome disruption and intestinal permeability — what’s often called the gut-thyroid axis — with autoimmune thyroid conditions including both Graves’ disease and Hashimoto’s thyroiditis. A compromised intestinal barrier may allow microbial antigens to activate immune pathways that cross-react with thyroid tissue. I address gut health when necessary or clinically indicated — including dietary anti-inflammatory strategies, targeted probiotic support, and evaluating for gluten sensitivity in susceptible patients.
Iodine Awareness
High iodine intake can worsen hyperthyroidism in Graves’ disease by providing additional substrate for excess thyroid hormone production. I advise patients to avoid high-dose iodine supplements and kelp or seaweed products while on antithyroid therapy. This is frequently missed — many patients arrive taking iodine-heavy “thyroid support” supplements purchased online that are actively working against their treatment.
Why You Should See a Board-Certified Endocrinologist for Graves’ Disease
Graves’ disease is not a condition to manage by trial and error. The antibody testing, treatment sequencing, dose titration, monitoring intervals, and decisions around remission versus long-term therapy all require endocrinology expertise — not just a basic thyroid panel from a primary care visit.
I trained at Mount Sinai and Albert Einstein and have spent over 20 years managing complex thyroid conditions. What that means for you, practically, is that I don’t just work to normalize your thyroid test results — I work to understand your entire endocrine/metabolic profile, and create a management plan that fits your life, not a protocol checklist.
If you’ve been symptomatic without a clear diagnosis, or if you’ve been diagnosed with Graves’ disease but don’t feel like your treatment is working, a second opinion from a specialist is always worth it.
What to Expect at Your First Visit
When you come to see me in Fairfield, CT, we’ll start with a thorough history — because Graves’ disease symptoms often overlap with anxiety disorders, cardiac conditions, and other hormonal imbalances, and getting the full picture is essential. We’ll review any labs you’ve had done, order the appropriate antibody testing if not already completed, and discuss what your thyroid ultrasound or uptake scan shows.
From there, we build a plan together — whether that’s starting antithyroid medication, discussing longer-term options, co-managing thyroid eye disease, or optimizing your overall metabolic and immune health alongside conventional treatment.
You deserve a provider who takes Graves’ disease seriously and manages it with the precision it requires.
Frequently Asked Questions About Graves’ Disease
Can Graves’ disease go into remission?
Yes. With antithyroid medication such as Methimazole, a number of patients can achieve clinical remission after 12–18 months of treatment. The remission rate varies — estimates range from roughly 10–30%, with higher rates seen in younger patients with a smaller goiter. Remission is not guaranteed, and many patients require long-term or indefinite therapy, which is also a safe and well-supported approach. This is always an individualized conversation.
Is Graves’ disease hereditary?
There is a strong genetic component. If a close family member has an autoimmune thyroid condition — whether Graves’ disease or Hashimoto’s — your risk is meaningfully higher. That said, genetics rarely act alone. Environmental triggers, including significant psychological stress, infections, and hormonal shifts such as postpartum changes, typically “flip the switch” in genetically susceptible individuals.
Do I have to stop exercising if I have Graves’ disease?
Not necessarily, but modifications are often appropriate. Until your heart rate and thyroid hormone levels are stabilized with medication, I typically recommend avoiding high-intensity interval training (HIIT) or heavy cardiovascular exercise to protect your heart. Once your levels normalize, a gradual return to full activity is usually well tolerated. I address this as part of every new patient plan.
What is the difference between Methimazole and Radioactive Iodine for Graves’ disease?
Methimazole (an antithyroid drug) works by blocking new thyroid hormone production while preserving the gland — it’s reversible and is now the preferred initial approach for most patients. Radioactive iodine permanently destroys thyroid tissue, resolving hyperthyroidism but typically resulting in lifelong hypothyroidism requiring thyroid hormone replacement. The right choice depends on your individual situation, including whether you have thyroid eye disease, are pregnant, or prefer to avoid radiation.
How do I naturally lower thyroid antibodies with Graves’ disease?
While antithyroid medication is the primary tool for controlling hyperthyroidism, evidence-backed complementary strategies can support immune regulation. Selenium supplementation, Vitamin D optimization, stress management, and addressing gut health when clinically indicated are all part of my functional approach. These do not replace medical treatment — but they address the immune environment that drives the disease, which conventional care alone often does not.
Looking for a Hyperthyroidism Specialist in Connecticut?
If you’re experiencing symptoms of hyperthyroidism or have been diagnosed with Graves’ disease and want expert endocrinology care in Fairfield, CT, I’d welcome the opportunity to work with you. Patients travel from across Fairfield County — Westport, Greenwich, Darien, Trumbull, and beyond — for a level of thyroid care that goes beyond the standard protocol.
My practice, Restore Health, is designed for patients who want more than a prescription — they want answers.